The Pfizer coronavirus vaccine is officially making rounds through the US. Healthcare workers and long-term care facility residents are first in line to receive the doses. There are other immunization options in development, too, with Moderna being the most prominent competitor.
While this news boosts hope, you might be apprehensive about receiving your shot. Let’s dispel some worries by examining what we know so far about these two options.
The Ingredients Are Similar
Both vaccines use messenger RNA as their main ingredient, which triggers your body’s immune response. The other elements are also quite similar. Also, at such small dosages, neither of the included chemicals is toxic or dangerous.
Pfizer
This treatment contains highly-purified mRNA, with the genetic code of a specific coronavirus part – the spikes all over its surface. However, these elements don’t stem from live cells, which makes them harmless. The oil (lipid) bubbles hold them, preparing your body for protein absorption.
The liquid part consists of saltwater, which maintains the treatment’s pH levels. That way, it’s easier for the body to accept the contents.
Moderna
This one also features COVID-19 spike protein mRNA. However, the company used the live virus genome as a template, reproducing it in a laboratory. Moderna also wraps the mRNA in lipids, protecting it as it enters your cells.
The solution is a bit different but serves the same purpose of matching the pH levels to our bodies.
Both Require Double Doses
Whichever vaccine you pick, you’ll get two shots. The two manufacturers require different periods between doses one and two, but scientists don’t see much significance in the variance.
The priming dose comes first, equipping the body for an immune response. Then the booster shot follows, activating the immunity.
Pfizer
The second shot takes place three weeks after the first. Each dose contains 30 micrograms of the vaccine.
Moderna
This company has subjects receive their two shots four weeks apart. Each carries 100 micrograms of vaccine, but the effects aren’t much different, even with over three times the portion.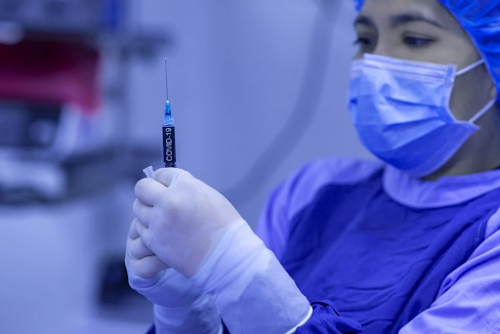
Both Are Mostly Effective
Both alternatives’ primary goal is to prevent symptomatic COVID-19, including coughing, fevers, and shortness of breath.
They show excellent efficiency in eliminating severe conditions and deaths. It’s still quite unclear whether they help with asymptomatic coronavirus, though.
Pfizer
Trials show that, after people receive the full vaccine dose, Pfizer is 95% effective at preventing symptomatic illness. However, no data related to asymptomatic infections or shedding rates after your vaccination exists.
Moderna
For now, the Moderna trials show 94.1% effectiveness at protecting people from coronavirus symptoms. Some preliminary evidence suggests that it could prevent asymptomatic infections, too, but the data is still too limited for specific conclusions.
Both Come With Light Side Effects
Large trials for both vaccines showed no harsh side-effects. The lighter ones are quite similar in both and resemble COVID-19 symptoms. Moderna’s could be somewhat stronger than Pfizer’s, though.
Either way, as HealthTap explains in its Covid Vaccine FAQ, doctors and experts believe both options are highly safe and effective.
Pfizer
Commonly noted side-effects are:
- Injection site pain
- Fatigue
- Headache
Regarding severe symptoms, they took place rarely and only after the second dose, including:
- Severe fatigue
- Severe headaches
- Severe chills
- Muscle pain
There was controversy, though, after some recipients experienced an allergic reaction following their shots. As this risk didn’t come up during phase two trials, researchers are yet to locate its source.
Moderna
While the side-effects were the same for the Moderna trial participants, they occurred more commonly. Notably, a higher number of younger subjects experienced fatigue, headaches, and muscle pain.
When it comes to more dangerous contraindications, they’re similar to Pfizer. However, 6% of participants also recorded joint pain.

Neither Comes With Certain Durability
Protection durability is among the most significant unknowns of either vaccine.
Both immunization studies followed participants for at least two months after they received full doses. However, apart from that timeframe, it’s unclear how long the protection lasts. The question of whether re-vaccination will become necessary is yet to get clear answers.
The best thing the researchers can do so far is to follow individuals who received treatment, studying their antibody count over the months to come.
No Reason to Refuse
There doesn’t seem to be much of a difference between the two immunization options available in the US. As the first population groups receive their shots, more information will become available to alleviate the general public’s stress surrounding the idea of getting vaccinated.
Either way, both seem like a good step forward in combating the coronavirus pandemic.
Interesting Related Article: “The Effect of COVID-19 Vaccine Distribution on Global Businesses“

