Multiple Sclerosis, also known as MS, has for many years, progressed uninhibited despite the best efforts of immunotherapy and some older forms of stem cell therapy and treatment. Oftentimes, the stem cell treatments that are proposed by medical clinics around the globe are still considered stem cell research and thus, not completely practical or applicable to real-life or severe cases of multiple sclerosis.
With the research and application conducted by clinics such as Swiss Medica, however, the groundbreaking use of stem cell therapy has been effective in many cases of MS. This statistic goes far to prove that however novel or controversial some aspects of stem cell research are; it is here to make lives better.
This article aims to go into great detail, all you need to understand about ongoing stem cell research and the treatment plans for MS that are currently available and how it all works. The article is broken down into the following segments and you can skip to any segment that most addresses the questions you have;
- Everything you need to know about MS, its pathogenesis and evolution
- Origin and introduction of stem cell treatments in MS cases
- Types and forms of human stem cells applicable for MS treatment and management
- Reasons behind the recorded efficacy of MS stem cell therapy
- Proven Steps for administering SCT for MS patients
- Medical costs associated with stem cell therapy
- Adoption and statistics rates backing stem cell research and therapy around the world
From the beginning of the article, it is important to state that every passing day, more grounds are broken for stem cell therapy and new knowledge is gained that can continue to help the medical field provide better healthcare to individuals facing unfavourable MS prognosis.
That said, let us dive deeper and understand the health condition that is Multiple Sclerosis.
Everything you need to know about MS, it’s pathogenesis and evolution
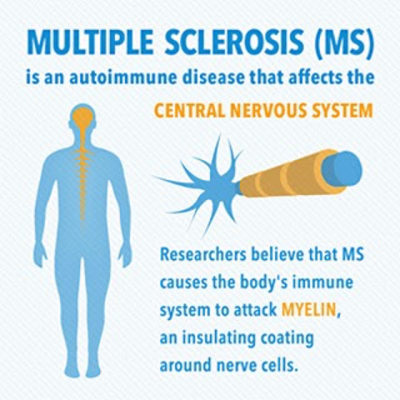
MS is a complex autoimmune disease of the central nervous system (CNS). In a healthy individual, there is a sheet of tissue that covers the nerves of the brain and spinal cord (the two major components of the CNS) which is called myelin and depending on factors ranging from nutrition, environmental exposure and even genetic factors, the myelin covering for your nerves can either be a thin or thick covering.
The MS problem arises when the body’s immune system responses attack this myelin and the cells that form it (known as oligodendrocytes) and disrupt its protective function for the nerves of the CNS, yielding the first stage of MS which is inflammation. The second phase of MS which is neurodegeneration occurs because the nerve cells no longer have that protective myelin covering.
MS is known to affect all ages of people but has been known to be first diagnosed when individuals are between the years of 15-40 years and MS is three times more prevalent in women than men. Although it has been mentioned that genetic factors play a role in the unique composition of the myelin in the brains of every individual, the onset of MS has been ruled as not being completely genetics-related.
Even when the immune system attacks its own myelin and myelin-forming cells, resulting in the relapse symptoms that are consistent with the first stages of MS, it is also shown that this first attack can be followed by complete regeneration of myelin and myelin-forming oligodendrocytes; a phenomenon which is known as remyelination.
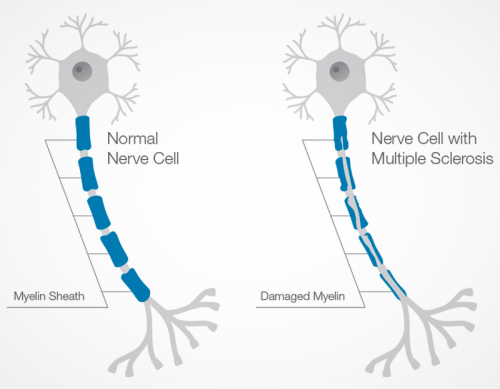
Although MS is best diagnosed by specialists, common symptoms have been identified based on the specific areas of the brain or spinal cord where the body’s immune cells attack the myelin coverings. These symptoms include:
- fatigue
- numbness
- muscle or leg twitches
- weakness and a general lack of coordination.
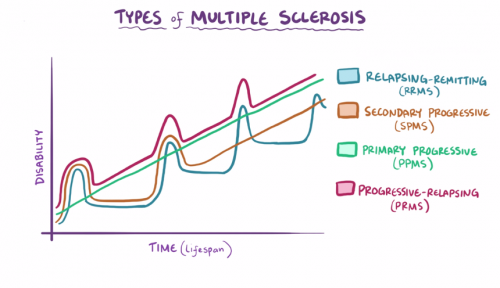
When categorized, MS is observed as showing mild to severe progressions and the four categories of MS that have been isolated from the most common to least common include:
- relapsing-remitting MS (RRMS)
- secondary progressive MS (SPMS)
- primary progressive MS (PPMS)
- progressive-relapsing MS (PRMS)
As the names of each category would imply, MS can either prevail in an individual by showing flare-ups of symptoms (relapses) and going into complete remission for long periods (RRMS) or continue progressing and worsening without chances of remission, as has been observed in the other three categories.
Origin and Introduction of Stem Cell Research for MS treatment
Following increasing isolation and understanding of the health condition, treatment options began developing and ranged anywhere from injectable medications to oral medications. In the beginning, these medications could only hope to suppress the actions of the body’s immune system and it was only a matter of time before the adverse effects of such immunosuppressants could be seen in other areas of the human body. Under different brand names, injectable treatments of interferon beta-1a and glatiramer acetate were administered as palliative measures since there are known cures for MS.
As more medical research was conducted and more details brought to light about the occurrence of MS, new models of treatment were proposed that could supplant the actions of immunosuppression and possibly give back to individuals a good chance at living out a high-quality life.
The result of this research for a new mode of treatment for Multiple Sclerosis? STEM CELL TRANSPLANTATION.
As soon as the pattern of the pathogenesis of MS was isolated and it was known that the body’s immune system was attacking the myelin covering of its CNS, it only seemed an angle worth exploring that in addition to suppressing the actions of the immune system, the oligodendrocytes that form the myelin can either be fortified to keep forming myelin after severe cases of flare-ups or relapses or deposits of whole B and T cells can be made directly into the bloodstream and immune system, thus replacing native immune cells that are not functioning optimally.
The only regenerative factor that could be isolated from the human body to achieve this were stem cells.
Types and forms of human stem cells applicable for MS treatment and management
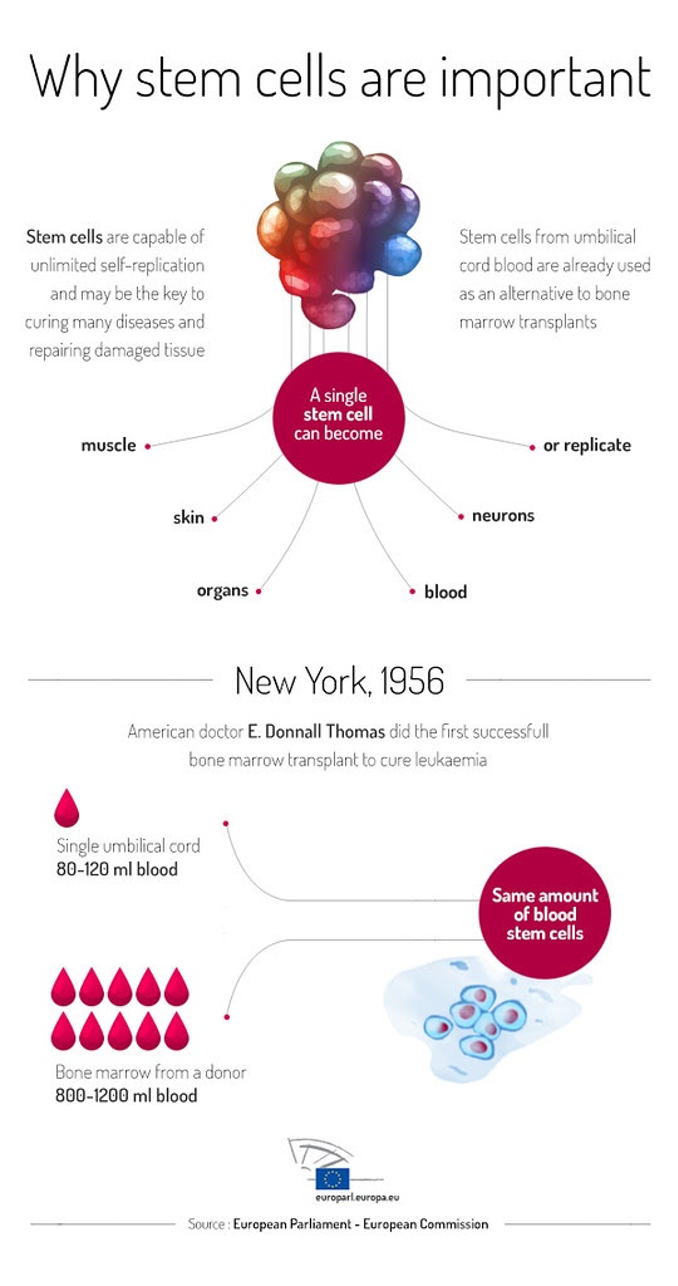
Typically, the body’s stem cells are an integral part of the body’s repair system and this feature, above all else, is why the MS treatment therapy that aims to apply it has been successful in many cases. If you’re looking for the most vivid way of imagining stem cells, think of newborn babies and how it is almost impossible to know certainly how they’d look when they grow up; stem cells can grow up to be any other kind of cell in the body in just the same way that babies can look different as adults than they did as babies.
Depending on what the body needs at a particular time, human stem cells can morph into nerve cells, red blood cells, immune cells or muscle cells.
As with the categories that Multiple Sclerosis has been split into to better understand it, the body’s stem cells have been categorized as human embryonic stem cells (hESCs), hematopoietic stem cells (HSCs), neural stem cells (NSCs) and induced pluripotent stem cells (iPSCs). Each type of stem cell is isolated and retrieved from specific parts of the body and constitute a separate form of stem cell therapy and the efficacy of their use has been shown to be competent to varying degrees in application to MS cases.
Reasons behind the recorded efficacy of MS Stem Cell Research
As you may have read earlier, the isolation and retrieval of stem cells for administration for health conditions including MS is especially efficient and successful because of the regenerative power of stem cells. As debilitating as MS is, the concept of the kind of research that can propose a treatment that causes the impaired cells of the body’s immune system to regenerate itself has been welcomed with hope and excitement.
Thus far, the most attention has been paid to the hematopoietic stem cell which is retrieved from the bone marrow and can differentiate into blood cells and cells of the immune system. HSC has received more research attention, not necessarily because it has the widest range of application but because it has unmistakable benefits without the ethical issues associated with, say, use of hESCs which require the use of human embryos.
At its core, stem cell therapy aims to treat MS in the most efficient manner possible by replacing the body’s ‘faulty’ immune system as it were or reboot it by replacing key immune cells, and correcting its propensity to attack its own cells, yielding lowered occurrences of inflammation and any subsequent neurodegeneration of the brain or spinal cord.
Proven Steps of administering SCT for MS Patients
Six Proven Steps are deployed for the application of the AHSCT (autologous hematopoietic stem cell transplantation) and is broken down thus;
- Identification and extraction of stem cell-containing fluids from MS patient’s bone marrow
- Infusion/Introduction of collected bone marrow components into the bloodstream (usually accompanied by immunosuppression through chemotherapy and introduction of synthetic growth factors (SGF) or granulocyte-colony stimulating factors (gCSF)
- A week or more later, blood samples are collected with a special machine and stem cells present are isolated and frozen to preserve for use in the later stages of AHSCT.
- Native immune cells involved in the auto-immune disease (MS) are completely or partially destroyed or killed by another round of chemotherapy
- Stem cells are reintroduced into your bloodstream through specially formulated drips. At this stage, the best-case prognosis is that new blood cells and brand new immunity can be generated by these stem cells within a month of their reintroduction in your bloodstream
- After the destruction and subsequent rebuilding of your immune system is complete with the fifth stage, the sixth stage is primarily a recovery stage. Susceptibility to infections and injuries during this stage is very high and thus, it is taken just as seriously as the other stages of stem cell treatment and transplantation, perhaps even more seriously.
Although the steps above show you the process for AHSCT, multipotent mesenchymal stem cells (MSCs) can be also used for MS treatment and these MSCs can either be autologous (i.e. extracted from the patient’s body) or extracted from a matching donor.
The advantage of MSCs for MS treatment is that they do not require chemotherapy, thus the treatment is more ‘natural’. In multiple sclerosis, these types of cells can be administered intravenously, intrathecally, or locally to achieve the desired result.
Medical Costs associated with receiving MS Stem Cell Treatment
As you may have surmised from the amount of time and painstaking process that stem cell therapy is, it is not a treatment that isn’t without steep costs. For every country, state or region, the cost of receiving the benefits and care that comes from extensive stem cell research for the treatment of Multiple Sclerosis will vary depending on economic, social and even political factors.
A number of medical considerations that go into every unique MS stem cell treatment can affect the total cost and this is so for the Swiss Medica Clinic where the following details are considered;
- the type of stem cells that will be administered (and by extension, the location for extraction and whether or not it’ll be autologous or donor-based)
- expansion of the stem cell cultures before administering (as well as the ease with which this expansion process is performed)
- distance from the nearest clinic
- the severity of MS progression (which determines the number of therapies to be administered to reverse the progression)
Anywhere from $7,000-$25,000 depending on the increasing complexities of your MS prognosis has been delineated as the most common industry cost but the best course of action will always be to contact medical advisers or request a call today to get the right information about your unique prognosis.
Adoption and Statistics Rates backing MS Stem Cell Research and Therapy
Although the application of stem cell transplantation for MS treatment has been widely adopted and is frequently proposed to individuals facing near-fatal prognosis, there are still steps taken to ensure that patients are getting the right treatment plans for MS which ensures that they witness successful outcomes. As of 2014, countries in North America and Asia such as the United States, Iran and South Korea were at the forefront of breaking new grounds for finding lasting stem cell treatments or complete cures for Multiple Sclerosis and since then, the number of participating countries has only increased and at every turn, information on new discoveries are being shared with the help of academic journals and conferences organized for that purpose.
In this 2017 study published in the JAMA Neurology journal, conclusions drawn from the observation of the long-term outcomes for MS patients who have successfully completed AHSCT transplantation showed that survivors (which was more than half of the observed population) were free of any neurological progressions even after 5 years.
The evaluations in this PubMed study show the effectiveness of transplantation of mesenchymal stem cells (MSCs) in immunomodulation and high chances of tolerability after MSCT. It also showed that whether mesenchymal stem cells were extracted from the patients (autologous) or from healthy donors, they showed similar proliferation and patterns of differentiation in vivo.
You can watch patient’s results after MS treatment with stem cells, shared on YouTube.
Above all else, early detection of MS has been the greatest determiner of the success of stem cell therapy in reducing ongoing clinical relapses and halting the progression of inflammatory symptoms of the auto-immune disease to neurodegeneration. Along with this fact, a younger age at the time of diagnosis or the first round of treatments, fewer incidences of prior immunotherapies and low disability scores were also important notes for the cases of MS that have been effectively treated at best or efficiently managed for the rest of a patient’s life.
Long before the discovery of the efficacy of stem cell research, it was believed that, at best, individuals diagnosed with MS could only hope to receive care that would make the degeneration of their CNS less unpleasant, and yet, the successes that have been recorded since the commercial use of stem cell treatments point to the reality that it can only get better as more time passes.
Interesting Related Article: “Clues to autoimmune origins of lupus in precursor cells, say researchers“

