Pressure is a standard parameter used to monitor vital signs of the body, especially that of the blood. Unknown to many, our eyes also have a measurable form of pressure, called the intraocular pressure (IOP). IOP is the fluid pressure within the eye. What makes IOP a vital parameter to measure and how does it affect vision?
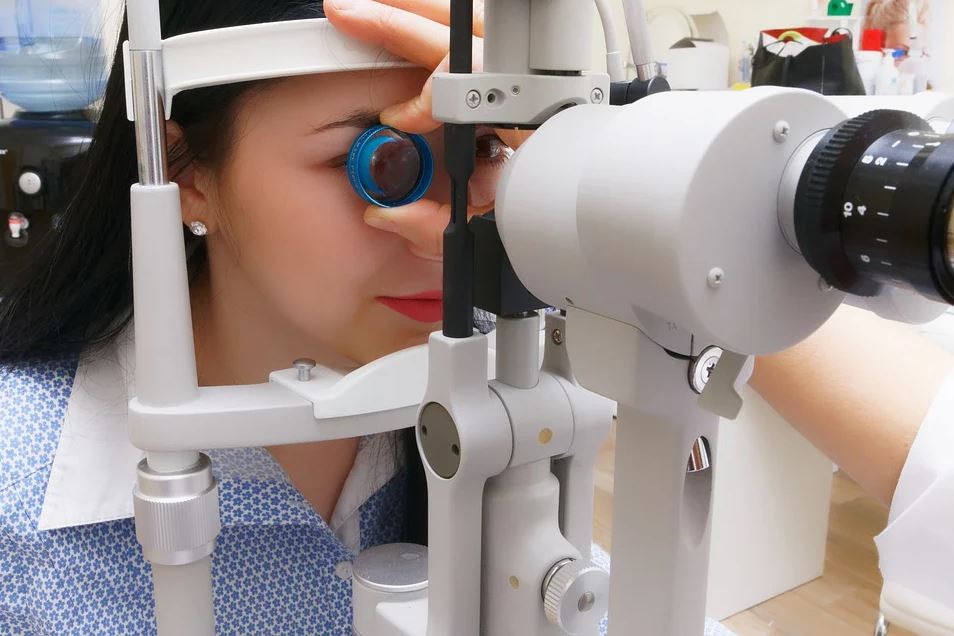
As mentioned earlier, the fluid inside the eye has a certain amount of pressure which can be measured by optometrists using a procedure called tonometry. A tonometer is used for this process and is calibrated to gauge eye pressure in millimeters of mercury (mmHg). You can learn more about this when you visit https://www.elitevisioncenters.com/.
There are several invasive and non-invasive methods to measure fluid pressure that you’re going to notice when you visit an optometrist. These methods differ when it comes to accuracy. The most widely accepted non-invasive method is Goldmann tonometry, wherein the tonometer uses a special prism that pushes lightly against the cornea. A spring determines pressure by aligning circles on a filter as force is applied from the tonometer.
However, applying force on the cornea can cause damage. Thus, the dynamic contour method was developed. The process uses a hollow tip that has the same curve as the cornea, and attached to its center is a small pressure sensor that can measure IOP 100 times per second. The change in pressure is calculated by a computer depending on the change in resistance of the piezoresistive sensor.
The widely accepted consensus among eye care specialists on the normal intraocular pressure is between 10 mmHg and 20 mmHg. Thus, the average IOP among adults is around 15.5 mmHg with a deviation of about 2.5 mmHg. Pressures below and above this range can have a significant impact on the eyes.
Ocular hypertension (OHT) occurs when a person’s IOP is above the normal range, which can lead to glaucoma. This disease arises due to damage to the eye’s optic nerves and may ultimately lead to vision loss if left untreated. People suffering from OHT may experience hazy or blurred vision, severe eye and head pain, and vomiting. Surgical techniques and medicine are available to reduce IOP and minimize the effects of glaucoma.
On the other hand, ocular hypotension or hypotony occurs when the eye’s IOP falls below 5 mmHg. Low IOP may indicate that the eye has fluid leakage, retinal detachment, or inflammation. The condition can also develop if the eye’s choroid layer (the layer between the sclera and retina) becomes detached or if the anterior chamber becomes shallower than usual. Optometrists employ various methods to promote fluid flow to correct loss of fluids, which includes suturing of the eye’s drain canals, patching, blood injection, and introducing substances to reshape shallow portions of the eye.
Intraocular pressure is an essential parameter that optometrists measure to prevent eye diseases. Visit your nearest optometrist now to determine your IOP, and effectively prevent disorders from developing.
You may be interested in: Hypertension: What Is It?

